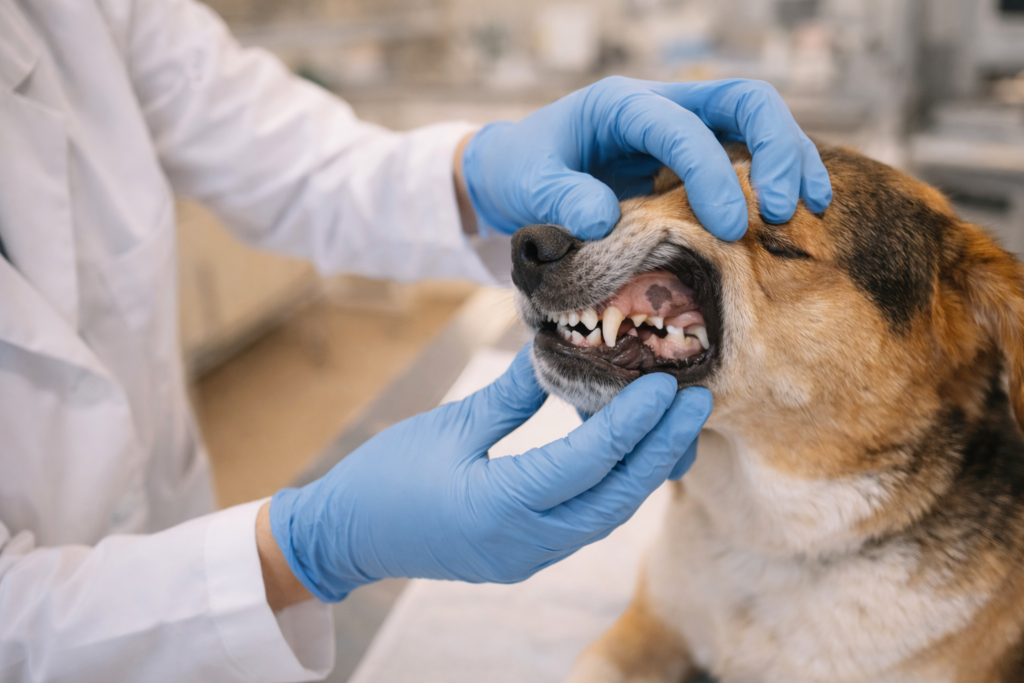
Most dog owners notice bad breath and assume it’s just one of those things that come with having a dog. They don’t connect it to anything serious. They might mention it at a vet visit, get a suggestion to try dental chews, and move on. But what’s actually happening beneath the gum line in a dog with untreated periodontal disease is considerably more serious than an unpleasant smell — and the consequences can reach far beyond the mouth itself.
This is a topic worth understanding in detail, because dental disease is the single most common medical condition in adult dogs. By the age of three, the majority of dogs have some measurable degree of it. And yet for many families, it remains low on the list of health priorities — often until a problem becomes painful, advanced, and much harder to address. If you’ve been searching for a dog dentist near you in Brampton or wondering whether your dog’s teeth actually need professional attention, this guide answers those questions honestly and thoroughly.
What Periodontal Disease Actually Is — and Why It’s Not Just a Dental Problem
Periodontal disease is an infection of the structures surrounding the teeth: the gums, the periodontal ligament, and the alveolar bone that anchors each tooth in its socket. It begins with plaque — a biofilm of bacteria that accumulates on the tooth surface after every meal. When plaque isn’t removed regularly, it hardens into tartar (also called calculus), which creates a rough surface where even more bacteria can colonize. As the bacterial load beneath and around the gum line increases, the body mounts an immune response to fight the infection. That immune response is what causes the swollen, red, bleeding gums we call gingivitis.
Gingivitis, if caught early, is reversible. But once the infection progresses past the gum line into the supporting structures of the tooth, the damage is permanent. Bone is lost. Teeth loosen. Abscesses form. And at every stage of this process, periodontal pathogens — the bacteria responsible for the infection — have access to the bloodstream through the inflamed, compromised gum tissue.
That bloodstream access is exactly where the story stops being purely dental and becomes a whole-body health problem.
The Systemic Connection: How a Mouth Infection Reaches the Heart and Kidneys
The mechanism by which oral bacteria cause harm elsewhere in the body is not theoretical — it’s been documented in both human and veterinary medicine for decades. When periodontal pathogens enter circulation through diseased gum tissue, they don’t stay local. They travel. And certain organs are particularly vulnerable to their effects.
The Heart
The connection between periodontal disease and cardiac conditions — particularly endocarditis (infection of the inner lining of the heart) and valvular disease — has been studied extensively in dogs. Bacteria from the oral cavity can attach to the heart valves and endocardium, establishing infection that impairs the heart’s ability to function normally. Small breed dogs are already predisposed to mitral valve disease as they age, and the presence of chronic oral infection appears to accelerate and exacerbate that process.
Systemic inflammation plays a central role here. The body’s chronic immune response to ongoing oral infection produces inflammatory mediators — including cytokines and C-reactive protein — that circulate throughout the body and contribute to tissue damage in the cardiovascular system. It’s the same general mechanism linked to heart disease in humans with chronic periodontitis, and the veterinary evidence increasingly supports a parallel relationship in dogs.
The Kidneys
The kidneys filter blood continuously, which makes them a primary target for circulating bacteria and the inflammatory proteins produced in response to infection. Chronic bacteraemia from periodontal disease creates a persistent low-grade burden on renal filtration that, over time, contributes to progressive kidney damage. Studies in dogs have found a statistically significant association between the severity of periodontal disease and markers of renal dysfunction — suggesting that the kidneys pay a genuine long-term price for untreated oral infection.
This is particularly important in ageing dogs, where some degree of kidney function decline is already expected. Chronic systemic inflammation originating from the mouth adds an avoidable additional load to kidneys that are already working harder than they were in youth.
The Liver
The liver, like the kidneys, processes circulating bacteria and their metabolic byproducts. Hepatic changes associated with chronic periodontal bacteraemia have been documented in veterinary medicine, typically presenting as elevated liver enzymes on bloodwork without obvious clinical signs until the condition is well established. It is another example of organ-level consequences that develop slowly, silently, and without any obvious connection to a dog’s dental status — until bloodwork makes the link visible.
The Stages of Periodontal Disease: A Comparison
| Stage | What’s Happening | Visible Signs at Home | Reversible? |
|---|---|---|---|
| Stage 1 — Gingivitis | Plaque and early tartar accumulation; gum inflammation without bone loss | Mild bad breath; gums may appear slightly red at the margin | Yes, with professional cleaning and home care |
| Stage 2 — Early Periodontitis | Up to 25% loss of tooth-supporting structures; early bone involvement | Noticeable bad breath; some bleeding on chewing; slight gum recession | Partially — bone loss is permanent but progression can be halted |
| Stage 3 — Moderate Periodontitis | 25–50% loss of attachment; deepened pockets; active infection present | Persistent bad breath; difficulty chewing hard food; possible pawing at face | No — management focuses on slowing progression and relieving pain |
| Stage 4 — Severe Periodontitis | Greater than 50% structural loss; tooth mobility; abscess formation likely | Visible tooth loosening; reluctance to eat; facial swelling possible; significant behaviour change | No — affected teeth typically require extraction |
The critical take-away from this progression is that stages 1 and 2 are the intervention window — the point where professional cleaning makes a meaningful difference and where the systemic consequences are still largely preventable. By stage 3 or 4, the damage done to the mouth is permanent, and the body has been dealing with chronic bacterial exposure for months or years.
Signs Your Dog May Have Dental Disease Right Now
Persistent or Noticeably Worsening Bad Breath
This is the most common first observation. Dog breath is never going to be fragrant, but a distinctly foul, rotten, or unusually strong odour — particularly one that seems to be getting worse over time — is a reliable indicator of active oral infection rather than normal bacterial baseline. If visitors comment on your dog’s breath before you do, that’s generally a signal worth acting on.
Changes in Eating Behaviour
Dogs in oral pain rarely stop eating entirely — their drive to eat is too strong. Instead, they adapt. They may drop food more often than usual, chew exclusively on one side of the mouth, prefer softer food, eat more slowly, or show hesitation before picking up a hard treat or toy. These changes are easy to attribute to age or preference without recognizing them as pain responses. Any noticeable shift in how a dog approaches food warrants a dental assessment.
Visible Tartar Accumulation
Brown or yellow-brown mineral deposits on the teeth — particularly along the gum line on the upper back molars and canines — are calcified plaque that cannot be removed by brushing at home. Their presence indicates that professional scaling is needed. Tartar is not simply an aesthetic concern; it harbours and protects the bacterial colonies driving the infection beneath the gum line.
Swollen, Bleeding, or Receding Gums
Healthy gum tissue is pale pink, firm, and sits snugly against the tooth. Gums that bleed when touched, look bright red or purple at the margin, or appear to be pulling away from the teeth are showing active inflammatory responses to ongoing bacterial challenge. These are not symptoms that resolve on their own.
Pawing at the Face or Rubbing the Muzzle
Dogs experiencing dental or facial pain will often try to address it themselves by pawing at the affected side or rubbing their face along the floor or furniture. This behaviour, particularly when it’s new or increasing, is a fairly direct signal of oral discomfort rather than a quirk.
Behavioural Changes — Irritability, Withdrawal, or Reduced Playfulness
Chronic pain changes temperament. A dog dealing with ongoing dental pain may become less engaged with play, less tolerant of handling around the face and head, more easily irritated, or generally quieter and less social than their baseline. These changes are frequently attributed to ageing rather than to a treatable pain source. A professional dental examination often reveals the cause.
What a Professional Veterinary Dental Visit Actually Involves
Many owners are unsure what to expect when they bring their dog in for a professional dental cleaning with a veterinary dentist or vet with dental capabilities — particularly around the use of anaesthesia. Here’s a clear picture of the process.
Pre-Anaesthetic Assessment
Before any procedure involving general anaesthesia, a thorough physical examination and pre-operative bloodwork are performed. This bloodwork screens for underlying organ conditions — including kidney and liver function — that could affect how the dog metabolises anaesthetic agents. At Lacoste Animal Hospital’s in-house diagnostic laboratory, these panels are processed on-site so the results are available the same day, allowing the procedure to proceed without unnecessary delay or off-site referrals.
Why Anaesthesia Is Non-Negotiable for a Real Dental Cleaning
This is a question that comes up often. Some facilities offer “anaesthesia-free” dental cleaning, which involves manually scaling visible tooth surfaces on a conscious dog. While it may appear thorough, it addresses only the supragingival (above gum line) surface of the tooth — and it’s the subgingival (below gum line) environment where the actual disease-causing bacterial load lives. A proper dental procedure requires the dog to be still, the mouth to be fully accessible, probing of every periodontal pocket, and the ability to take intraoral radiographs to assess root and bone health. None of that is possible without general anaesthesia. A legitimate vet dentist or veterinary dental practitioner will always insist on this standard of care.
Scaling, Polishing, and Probing
Under anaesthesia, the veterinary dentist uses ultrasonic scaling equipment to remove tartar from all tooth surfaces — above and below the gum line. Each tooth is then polished to smooth the enamel surface, which reduces the rate of future plaque adhesion. The periodontal pocket depth around every tooth is recorded with a probe, and digital intraoral radiographs are taken to assess the health of the tooth root and surrounding bone in areas not visible to the naked eye. If tooth extraction is necessary — for teeth with irreversible bone loss or abscess formation — this is performed during the same visit with appropriate pain management.
At Lacoste Animal Hospital Brampton, dental health is assessed as part of every wellness exam, and professional cleaning recommendations are made based on each dog’s individual presentation rather than a blanket protocol. If you’ve been meaning to have your dog’s teeth looked at and have been searching for a dog dentist near you in the Brampton area, the clinic serves the full Peel Region.
At-Home Dental Care: What Makes a Difference Between Professional Visits
Professional cleaning addresses the current state of the mouth — it removes existing tartar and treats active disease. What happens between professional visits determines how quickly the problem returns. At-home care is therefore not optional if the goal is to actually maintain dental health rather than simply address it in cycles.
Daily tooth brushing with a dog-specific enzymatic toothpaste is the single most effective at-home intervention. The mechanical action of the bristles disrupts the plaque biofilm before it can mineralise into tartar. Two or three times weekly provides meaningful benefit if daily is genuinely impractical. Human toothpaste should never be used — it contains fluoride and xylitol, both of which are toxic to dogs.
Dental chews, water additives, and prescription dental diets can serve as supportive measures but are not substitutes for brushing. They reduce plaque accumulation modestly but do not address subgingival pockets, where the disease process is most active. The Veterinary Oral Health Council (VOHC) seal is a useful guide when evaluating commercial dental products — it indicates the product has been tested and shown to have measurable efficacy.
How Often Should a Dog See a Veterinary Dentist?
For most dogs, an annual professional dental examination with cleaning as clinically indicated is the standard recommendation. Certain factors increase the frequency with which a dog is likely to need professional intervention:
Small and toy breeds accumulate tartar faster than large breeds and often have more crowded dentition, which creates additional pockets for bacterial accumulation. Brachycephalic breeds (flat-faced dogs like pugs, bulldogs, and shih tzus) have compressed jaw structures that present particular dental challenges. Dogs who receive no at-home dental care between visits will develop significant tartar much faster than those who are brushed regularly. And dogs with a history of moderate to severe periodontal disease typically need more frequent monitoring — every six months in some cases — to stay ahead of recurrence.
Your veterinarian’s assessment at each wellness exam is the most accurate guide to your individual dog’s frequency. What the data from those exams show over time is more informative than any general guideline.
A Note on Dogs Who Are Already Showing Systemic Changes
Sometimes the connection between dental disease and systemic organ changes isn’t discovered until bloodwork done for another reason reveals elevated liver enzymes, markers of early renal dysfunction, or an unexpected cardiac finding during a physical examination. In those cases, a thorough dental assessment often becomes part of the diagnostic picture — because unresolved oral infection can actively contribute to what’s happening elsewhere in the body.
At Lacoste Animal Hospital Brampton, the integration of wellness exams, in-house bloodwork, and dental assessment means these connections get made rather than missed. The post on the top signs your pet needs preventive care covers the full range of systemic indicators to watch for, many of which trace back — at least in part — to oral health status. And for a broader picture of the clinic’s diagnostic capabilities, our overview of a day in Lacoste’s diagnostic centre is worth reading.
Frequently Asked Questions
-
My dog is eating fine and seems happy. Does he really need a dental cleaning?
Yes, and this is one of the most common misconceptions in veterinary dentistry. Dogs are exceptionally good at masking oral pain — they continue eating through significant discomfort because the drive to eat is stronger than the pain signal. Appearing happy and eating normally is not the same as being pain-free. Regular dental assessment by a vet dentist is the only way to accurately evaluate what’s happening beneath the gum line.
-
Is anaesthesia safe for my older dog?
Modern anaesthetic protocols, combined with thorough pre-anaesthetic bloodwork and continuous monitoring throughout the procedure, make general anaesthesia considerably safer than it was even a decade ago. The greater risk for most senior dogs is actually leaving significant dental disease untreated — because the ongoing bacteraemia and systemic inflammation from active periodontal infection place real burdens on the heart, kidneys, and liver over time. The decision is best made in consultation with your veterinarian after reviewing your specific dog’s bloodwork and health status.
-
Can I brush my dog’s teeth if he won’t let me?
Most dogs can be trained to accept tooth brushing with gradual desensitisation — starting by simply allowing you to handle their lips and gums, then introducing the toothpaste flavour (most are poultry or beef-based), then the brush. The key is patience and very short sessions with positive reinforcement. Your veterinary team can walk you through a practical approach during your next visit.
-
How do I know if my dog’s bad breath is dental disease or something else?
Most persistent bad breath in dogs is dental in origin, but certain odour qualities can point to other conditions. A sweetish or fruity smell can indicate diabetes mellitus. A urine-like or ammonia-tinged odour may reflect compromised kidney function. A genuinely rotten or necrotic smell typically indicates active periodontal infection or oral tissue necrosis. Any significant change in your dog’s breath warrants a veterinary assessment to identify the source — both dental and metabolic causes are clinically important.
-
Does Lacoste Animal Hospital provide dental services for dogs?
Yes. Dental health assessment is included in every wellness examination at Lacoste Animal Hospital Brampton, and professional dental cleaning is available as part of the clinic’s veterinary care services. The team works with Trupanion and Petcard for families managing the cost of veterinary procedures. To book a dental assessment or wellness visit, call +1 (905) 913-8888 or email petcare@lacosteanimalhospital.ca.
Taking Dental Health Seriously Before the Signs Become Obvious
The frustrating reality of periodontal disease is that by the time most owners notice the visible signs — the obvious tartar, the significant behaviour change, the facial swelling — the condition has usually been developing for months or years. The periodontal pathogens responsible for the infection have had extensive access to the bloodstream throughout that window, and the organ-level consequences of that chronic exposure are often already under way.
The good news is that this is one of the most preventable trajectories in companion animal medicine. Annual wellness exams with dental assessment, professional cleaning when indicated, and consistent at-home dental care between visits together form a straightforward protocol that meaningfully changes the odds. It doesn’t require finding a specialist or travelling to a dog dentist in Toronto — it requires a relationship with a vet clinic in Brampton that takes dental health seriously as part of whole-body preventive care.
If your dog hasn’t had a dental assessment recently — or if anything in this guide sounds familiar — the team at Lacoste Animal Hospital is available six days a week with extended evening and weekend hours.
Lacoste Animal Hospital Brampton
117, 50 Lacoste Blvd, Brampton, ON L6P 3Z8
Phone: +1 (905) 913-8888
Email: petcare@lacosteanimalhospital.ca
Hours: Mon 10 AM–9 PM | Tue 9 AM–7 PM | Wed Closed | Thu 9 AM–7 PM | Fri–Sun 12 PM–10 PM